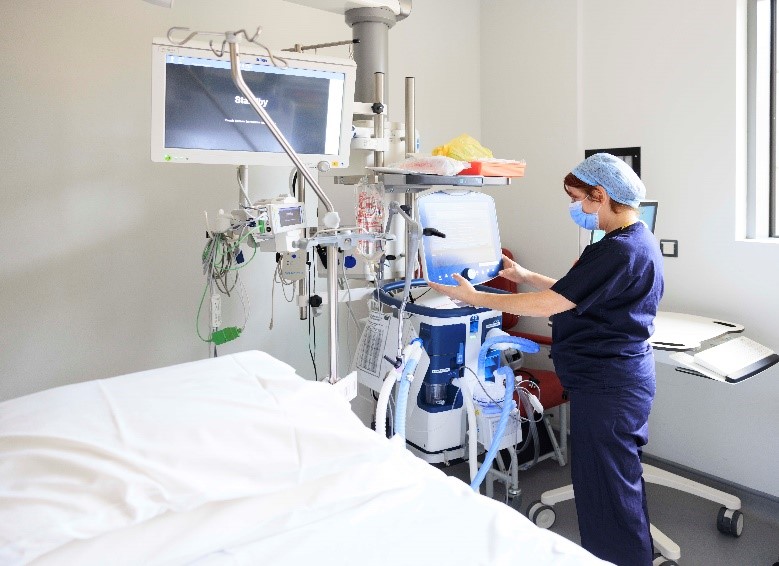
Our Intensive Care Unit is a 21 bedded unit where 15 of the beds are isolation rooms. Each room is fitted with the latest technology and equipment needed for patients requiring intensive care.
To care for a patient in Intensive Care they are attached to monitors that tell the team caring for your loved one what their heart rate is, their blood pressure, temperature and oxygen levels are.
All monitors and other equipment have visual and audible alarms. The alarm is designed to attract the attention of the nurse for a variety of reasons and does not necessarily mean there is a problem.
Many patients, especially if they have had major surgery, may need to use a ventilator (breathing machine) to help with their breathing. The patient is attached to the ventilator via a tube in the mouth, nose or throat. Patients are not able to speak while the tube is in place but speech should return to normal once the tube is removed. Patients on ventilators receive sedative and pain control drugs to make sure they are as comfortable as possible.
Patients that are sedated can look like they are asleep, but many at some level can still hear and relatives are encouraged to speak to the patient as reassurance and encouragement are proven to help with their recovery.