This incorporates medicines procurement and management, distribution of medicines to clinical areas, non-aseptic (extemporaneous) compounding and dispensing services for in-patients, day-case patients, patients attending the emergency department and clinical trial medication. We run a busy clozapine out-patient dispensing service. A Medicines Management Technician (MMT) service is currently provided on ten adult in-patient wards.
|
Our MMT service has demonstrated improved medicines supply and management of medicines at ward level. All pharmaceutical technicians providing the MMT service have undertaken or are in the process of completing additional training in medicines management.
The service involves: - MMT visiting the ward each week-day
- Ordering of both stock and non-stock medications for all in-patients
- Charging all medications on Cliniscript at ward level, and sending picking list to the dispensary printer via Wi-Fi
- Medications are supplied in the original packs without patient names, with some exceptions e.g. methotrexate, blood products, vaccines etc.
- Medications being put in the individual patients slots in the drug trolley by the MMT
- All non-stock medications ordered outside of the MMT service e.g. evenings and weekends are labelled with the patient identifiers.
The MMT service has resulted in improvements including: a. Average length of time per drug round was reduced by 20% at 8.15am and 16% at 11:30am with the introduction of a MMT. This equates to nine hours of saved nursing time per ward per week. The number of interruptions per drug round was reduced by 23% at 8:15am and 22% at 11:30am.
b. The percentage of missed doses due to unavailable medications was reduced from 2.98% to 1.62%- a 45% improvement.
c. Nurses agreed that the service led to an improvement in the time taken for medications to arrive to the ward after ordering
d. Improved endorsement of the Prescription Chart with location of medicines which is helpful to nurses.
e. Easier to for nurses to find medications on the ward 
|
 The aseptic unit is located in a clean room environment which must adhere to Good Manufacturing Practice standards. This unit is run by a dedicated team of highly skilled pharmacists and technicians. All chemotherapy, clinical trials for cancer patients and high cost/high risk products for gastroenterology/rheumatology departments are prepared under validated sterile conditions. In order to maintain these conditions, the aseptic unit is constantly audited against various standards. We work closely with our consultants and nursing staff to ensure the safe and efficient supply of treatment to our patients. We are involved in the development of protocols, policies and procedures for the safe administration of chemotherapy. .jpg)
Process improvement projects are ongoing in the aseptic unit and these are managed by dedicated pharmaceutical technician and pharmacists and discussed on a monthly basis at staff meetings. Staff receive continuous training and attend relevant in-house & UK training courses to maximise skill mix and support advanced roles. 
In order to manage workload a capacity plan is in place. 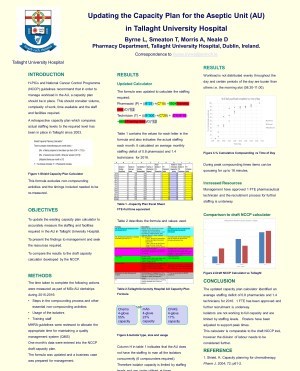
Systems which allow more efficient workflows have been introduced such as dose banding. 
|
Our Department is affiliated to the TCD School of Pharmacy & Pharmaceutical Sciences and we have an extensive programme of undergraduate, pre-registration and postgraduate education and training, as well as doctoral and post-doctoral research. This affiliation with TCD School of Pharmacy was formalised in 2015 with the signing of a Memorandum of Understanding. At any given time the pharmacy is training two pharmacy interns and two pharmacists are participating in the MSc in Hospital Pharmacy with Trinity College Dublin. We are the first hospital in our jurisdiction to have pharmacists complete a prescribing course in Queen’s University, Belfast, with four Tallaght University Hospital pharmacists completing the course since 2015. Pharmacists are involved in ongoing teaching for undergraduate and postgraduate pharmacy, nursing and medical students. Advanced Roles Training. PACT pharmacists: The extra responsibility and judgement required to deliver PACT led to the requirement that a PACT pharmacist has three years post-registration clinical pharmacy experience, a postgraduate qualification in hospital or clinical pharmacy and completes a training and validation programme. If you would like to learn more, see attached poster Collaborative Pharmaceutical Care At Tallaght University Hospital (PACT) - Development of Competency Training and Validation Programme. Our pharmacy technicians also complete externally validated advanced role in training in e.g. Medicines Management and In-Process Checking. We were the first Hospital in Ireland to employ a Research Pharmacist at Doctoral level. We have a well-established programme of bench research in collaboration with the Intensive Care Unit and the Department of Microbiology, on the pharmacokinetics of various antimicrobial agents during Continuous Renal Replacement Therapy. This research is done to improve patient outcomes through more precise dosing. We have a major practice research programme studying the impact and effectiveness of new models of clinical pharmacy service delivery. In 2014 we published our practice-changing paper Collaborative Pharmaceutical Care in an Irish Hospital and during 2015 we rolled out the new service model known as PACT, described below. We consider that this development epitomises the value and influence of research in our practice setting, in moving us to provider a safer, better service to patients.
|
The Hospital Drugs & Therapeutics Committee (DTC) provides overall governance of the medication use process in the hospital. The goals is assure the provision of safe, effective medication treatment within the available resources of the Hospital. Governance is shared by the leadership of the three key disciplines – Medical, Nursing and Pharmacy. In line with best quality management principles, these disciplines took a process-driven rather than a departmental approach and agreed at the outset to share governance of all policies, procedures and guidelines involving medication use. This has operated successfully since the Hospital opened. The DTC meets six times per year and uses a set agenda structured in line with the medication use process that reflects the elements of oversight: Formulary Issues, Financial Accountability, Medication Safety, and Medication Process Issues. In 2017 the DTC reviewed almost 200 documents in support of over 70 submissions: applications for new drugs to be added to the formulary; hospital policies, procedures, protocols and guidelines relating to medicines; collaborative practice agreements for nurse-prescribers. The committee’s review and input prior to approval is a means of ensuring delivery of safe, effective, evidence-based care. The DTC is a respected authority on medication use in the Hospital and reflects the principles of high co-operation, inter-departmental bridging and sharing of risks.
|
The Tallaght University Hospital Adult Medicines Guide is the operational framework to guide optimal medication use in the treatment of our patients. Evidence-based clinical guidelines are accepted by consensus and updated as needed. The purpose of the Guide is to enhance medication safety, promote use of recommended/ formulary drugs, and to ensure optimum use of resources. The Guide is available in book form in all clinical areas, as a mobile phone app, and as a desktop version on all PCs in the hospital. In the latter part of 2017, the Formulary Development Pharmacist co-ordinated a complete update of the Adult Medicines Guide. A team of almost 100 pharmacists, doctors, nurses, and dietitians worked on a collaborative basis to produce the 2018/19 edition. Each section is approved by at least one consultant in the area, meaning that end users can be confident that the Guide reflects international and local best practice.
|
The Medication Safety Programme has fostered a safety culture among the medical, nursing and pharmacy staff, as well as hospital management. We operate a non-punitive system of reporting of incidents and near misses in the hospital with a view to learning from being open about mistakes and taking preventive action against future harm. A high level of reporting is indicative of a positive safety culture. In addition to this, all nurses, doctors and pharmacy staff are required to complete the Online High Risk Medication Safety Training Course which is free to all hospital staff, and the system allows us to follow up on compliance. In this way we train the messengers who will bring us the safety signals we need to learn about our weaknesses and to address them where possible.
|
The Pharmacy Department’s mission is to ensure safe, efficient, cost-effective use and high quality use of medications by patients attending the hospital, through collaboration with nursing and medical colleagues. It is one of the busiest pharmacies in the country (See link to activity). Our dispensary stocks about 4,000 medicines. As well as dispensing over 300,000 prescriptions each year, we prepare 12,000 doses of chemotherapy and other intravenous medications in our Aseptic Unit. The Department is organised in a divisional structure to facilitate medication procurement, preparation and supply; clinical support for prescribers and nursing staff; medication policy development for the Drugs &Therapeutics Committee; and medication-related risk management including incident report processing, incident investigation, and improvement projects to enhance safe use of high alert medications. If you are admitted to hospital, our clinical pharmacists review your medication history to ensure continuity of care and to prevent errors. Pharmacists continue to play a very important role in your care time in hospital, working as part of the medical teams to ensure you get the best possible treatment, and to make sure you are discharged home smoothly. We aim to make sure that when you are discharged, your GP will receive a full report on your care within 48 hours, including your up to date list of medicines highlighting any changes that may have been made during your admission. We transmit this information electronically to GPs who have the Health link system. Teaching and Research are an important part of our role. We are affiliated to the School of Pharmacy & Pharmaceutical Sciences at Trinity College Dublin and twelve of our pharmacists hold official appointments at the University. We teach pharmacy students at undergraduate and post-graduate level as well as training Pharmacy Interns in the pre-registration year. Our research programme is designed to provide us with knowledge about the way medicines are used in the Hospital, so that we can change practice in order to do a better job for you, our patients.
We see our research as the bridge from today’s good practice to tomorrow’s better practice. Everyone in the department is committed to following the evidence that research provides. This can mean having to make big changes to the way we work. In 2015, led by the results of our research, we completely re-aligned the clinical pharmacists and started them working more closely with the medical staff in their teams, instead of the old way, which was to have pharmacists attached to wards. We are committed to patient safety and this year, with the support of the Hospital CEO, we launched a campaign called Zero Harm: Know Your Medicines, Part of this programme aims to assist you, the patient, with managing your medication throughout your admission, hospital stay and discharge.
|
Clinical pharmacists work at both multi-disciplinary team (MDT) level and in a number of specialities including intensive care, haematology, oncology, psychiatry, paediatrics, microbiology and clinical trials. The pharmaceutical model of care in place is known as the PACT model1 and it focuses on ensuring medication reconciliation is carried out at the point of admission and discharge to ensure the safe transition of patients in and out of the Hospital. Medication reconciliation is the process of ensuring that a patient is prescribed the most accurate list of medications a patient was taking prior to arriving in/leaving the Hospital and correcting any discrepancies identified. In addition, this model of care enables Clinical Pharmacists to collaboratively prescribe medications on the inpatient kardex to ensure the prompt resolution of medication discrepancies. Clinical Pharmacists will often participate in ward rounds and attend multidisciplinary team meetings where they offer their pharmaceutical expertise. Pharmacists visit patients at ward level and are involved in many aspects of patient care including drug usage review, promotion of safe, effective and economic medication use, patient and staff education, research, therapeutic drug monitoring, and other ward based clinical activities. Some of our Clinical Pharmacists see patients in the Atrial Fibrillation Clinic and will advise on the choice of drug/dosing/interactions as well as providing counselling to patients newly commenced on DOACs (blood thinners).
This clinic is the first of its kind in Ireland. 1. Grimes TC, Deasy E, Allen A, O'Byrne J, Delaney T, Barragry J, et al. Collaborative pharmaceutical care in an Irish hospital: uncontrolled before-after study. BMJ Qual Saf. 2014;23(7):574-83.
|